Eardrum Surgery Cost: Average Price, Factors, and Insurance Coverage
“Hearing-related surgery” can feel stressful enough—then the bills and insurance details add another layer. In most cases, eardrum surgery refers to repairing a hole (perforation) in the eardrum through a myringoplasty or tympanoplasty. Sometimes surgeons also repair the tiny middle-ear hearing bones (ossicles), which can change both the plan and the price.
If you’ve been searching for the eardrum surgery cost, you’ve probably noticed huge ranges. That’s normal: pricing depends on procedure complexity, the facility, your region, and what’s included (or billed separately). A helpful way to think about it is like pricing a home repair: the “project” might share the same name, but the final total depends on what’s actually found and fixed once work begins.
Most importantly, your final cost depends on your diagnosis and your insurance benefits—not just a posted “price.”
To learn more about what the procedure itself involves, you can also read our guide on how ENT surgeons repair a perforated eardrum: https://sleepandsinuscenters.com/blog/how-ent-surgeons-repair-a-perforated-eardrum
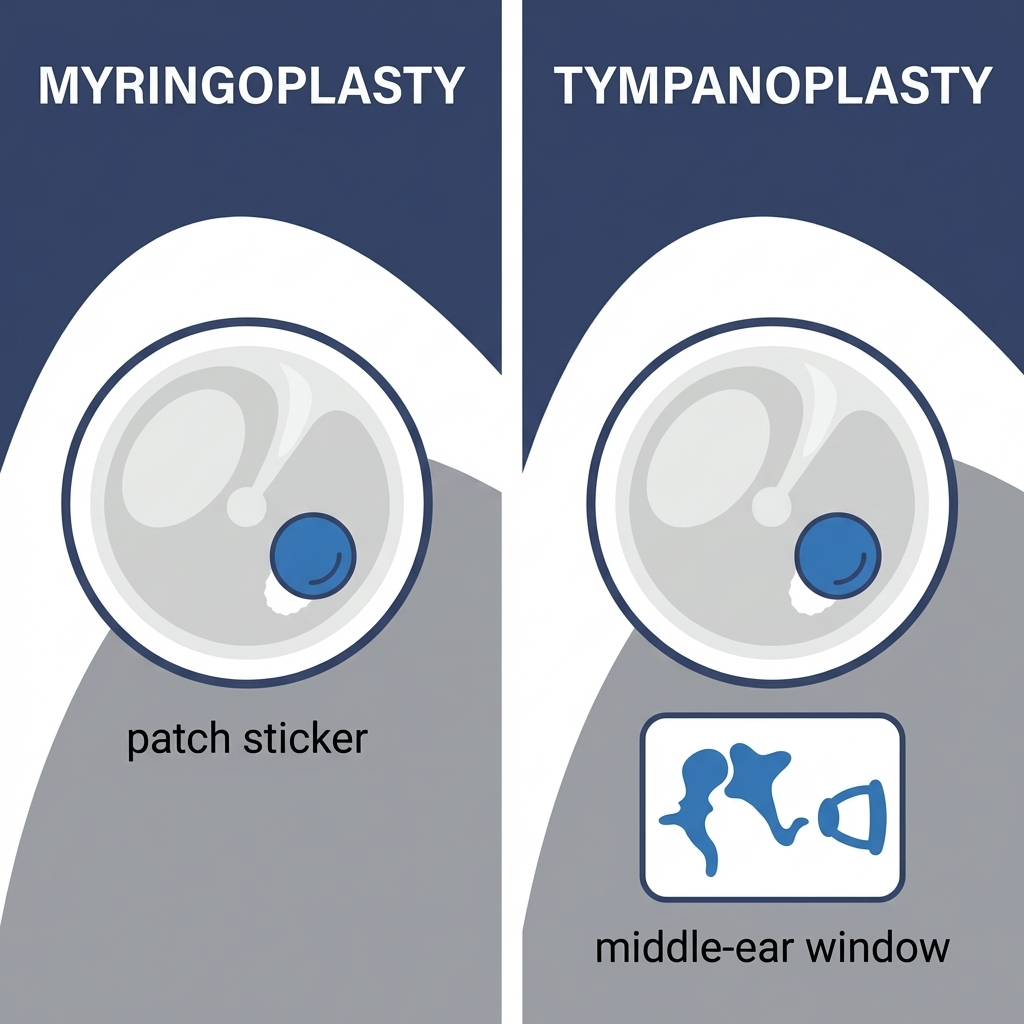
What Is Eardrum Surgery (And Which Procedure Do You Need)?
Myringoplasty vs. tympanoplasty (simple repair vs. repair plus middle-ear work)
- In many clinical settings, myringoplasty refers to repairing the eardrum (closing a perforation) without additional middle-ear reconstruction.
- Tympanoplasty generally refers to repairing the eardrum and evaluating the middle ear, with possible reconstruction if needed.
Because tympanoplasty may involve more steps, tympanoplasty cost is often higher than myringoplasty cost, even before you factor in anesthesia, facility fees, and follow-up testing. Usage and coding can vary by surgeon and institution, so ask your ENT how they’re defining and coding your procedure.
“Myringoplasty seals the ‘drumhead.’ Tympanoplasty seals it and checks the ‘room behind the drum.’”
When ossicular reconstruction (ossiculoplasty) is added
Behind the eardrum are three tiny hearing bones (ossicles) that help conduct sound. If these bones are damaged—sometimes from chronic infection or other middle-ear disease—your surgeon may recommend or perform ossicular reconstruction (ossiculoplasty).
This can increase eardrum repair surgery cost because it may involve:
- More operating time and surgical complexity
- Specialized instruments and materials
- A possible implant/prosthesis (which may be billed separately)
Some decisions depend on what the surgeon sees in the middle ear during the operation, which is one reason estimates can be hard to predict ahead of time.
Summary: The exact procedure—and the cost—often depends on what your surgeon finds in the middle ear at the time of surgery.
Symptoms That Often Lead to Eardrum Repair
Common symptoms of a perforated eardrum or chronic middle-ear issues
People often seek evaluation for symptoms such as:
- Reduced or muffled hearing
- Recurring ear drainage
- Frequent ear infections
- Pressure or “fullness”
- Ringing (tinnitus)
Some of these symptoms overlap with other middle-ear conditions. For example, fullness and muffled hearing can occur with fluid behind the eardrum—even without a persistent perforation. If you’re dealing with persistent fullness or hearing changes, this related overview may help you understand common causes and next steps: https://sleepandsinuscenters.com/blog/chronic-ear-fluid-and-hearing-loss-causes-symptoms-treatment
Summary: Similar symptoms can come from different problems, so a focused ENT evaluation helps match the treatment to the cause.
Red flags that need urgent care
Educationally, it’s helpful to know the signs that typically warrant prompt evaluation, such as:
- Sudden, significant hearing loss
- Severe pain with fever
- Dizziness/vertigo
- Facial weakness
If these symptoms are sudden, severe, or worsening, seek urgent or emergency care as appropriate; if you’re unsure how urgent it is, call an ENT office for guidance or follow local emergency instructions.
Summary: When in doubt with sudden or severe symptoms, err on the side of urgent evaluation.
Causes of Eardrum Damage (Why Surgery Might Be Recommended)
Infection-related causes
Eardrum perforations and middle-ear damage may be associated with:
- Recurrent ear infections
- Chronic fluid/inflammation in the middle ear
- Ongoing drainage that doesn’t resolve
A practical cost-related point: when infection or chronic inflammation is part of the picture, the surgeon may need to address more than “just the hole,” which can influence both procedure selection and total charges.
Non-infection causes
Other common contributors include:
- Trauma (including accidental injury from cotton swabs)
- Barotrauma (pressure changes from flying or diving)
- Prior ear tubes (some perforations persist after tubes)
- Blast injury/loud pressure-wave exposure
Even when the cause is straightforward, the size and location of the perforation—and the health of surrounding tissue—can still affect how complex the repair is.
Summary: The “why” behind a perforation matters less for price than the size, location, and overall ear health.

Average Eardrum Surgery Cost (U.S. vs. UK vs. Turkey Medical Tourism)
Important note: “Price” can mean very different things—hospital charges vs. insurer reimbursement vs. a bundled international package. Use the ranges below as reference points, not quotes.
United States cost range (often the highest)
In the U.S., listed facility charges for tympanoplasty-related procedures can land around approximately $10,200 to $20,800, depending on the procedure code and complexity (VA Outpatient Facility Charge Table, 2023) [1]. These are listed facility charges—not negotiated insurance rates, not total episode-of-care costs, and not the same as what patients pay out of pocket.
What you personally pay often depends on:
- In-network vs. out-of-network coverage
- Your deductible and coinsurance
- Whether anesthesia, implants, pathology, hearing tests, and follow-ups are billed separately
Concrete example: two patients might both have “tympanoplasty,” but one has already met their deductible (lower out-of-pocket), while the other has a high deductible early in the year (higher out-of-pocket). Add a separate anesthesia bill or an implant charge, and the totals can diverge quickly. This is why two people can have the “same” surgery yet a very different eardrum surgery price. Some sources also report U.S. estimates around $8,500 for tympanoplasty, though methodology and included services vary widely [3].
Summary: In the U.S., headline “prices” are often facility list charges—your out-of-pocket depends far more on benefits and network status.
United Kingdom private-care fee schedules (often lower list prices)
Some UK private fee schedules list examples such as:
- Myringoplasty: £663
- Combined-approach tympanoplasty: £753
(National Friendly Schedule of Fees, 2023) [2]
These amounts may reflect surgeon fees only and may not include anesthesia, facility, imaging, testing, or follow-up care. If you’re comparing, confirm whether the number represents the surgeon’s fee alone or a broader episode of care.
Summary: UK private “fees” often list just the surgeon’s charge, not the whole episode cost.
Turkey medical tourism packages (bundled pricing can look much lower)
Medical tourism listings commonly advertise tympanoplasty package pricing around approximately $2,500–$3,200 [3]. These are advertised package prices that may include select services (for example, surgeon, hospital, and airport transfers). Follow-up care, complication management after you return home, and unexpected added services may not be included—key factors when comparing totals.
Summary: Bundled packages can be appealingly low, but verify what is and isn’t included after you go home.
Why these numbers aren’t apples-to-apples
A major reason eardrum surgery cost varies so widely across countries is that you’re often comparing:
- “Charges” vs. negotiated insurance rates vs. all-inclusive bundles
- Different definitions of what services are included
- Differences in staffing, regulation, overhead, and follow-up norms
In other words, the headline number can be real—and still not represent the same set of services.
Summary: Always ask what the number includes before you compare it.
What Drives the Cost of Eardrum Surgery?
Procedure complexity (biggest driver)
Costs often rise when surgery involves:
- Larger or more complicated perforations
- Chronic infection or additional disease requiring more work
- Added procedures like ossiculoplasty (raising ossiculoplasty cost)
Think of complexity as the difference between patching a small tear versus rebuilding part of a structure: the name of the procedure may sound similar, but time, tools, and materials can change.
Surgical technique and technology
Costs can also vary by:
- Endoscopic vs. microscopic approach (often surgeon- and case-dependent)
- Graft material choices
- Use of implants/prostheses if reconstruction is needed
Even when technique differences don’t change outcome expectations, they can affect operating time, equipment, and billing categories.
Facility type and setting
Where you have surgery matters. A hospital outpatient department may have higher facility fees than an ambulatory surgery center due to overhead and contracting differences. If you’re comparing estimates, ask whether the quote is tied to a specific location (hospital vs. surgery center). The facility line item is often one of the biggest “swing factors.”
Provider and geographic region
Surgeon fees and facility pricing vary by region and local market. In many areas, metro regions tend to be priced higher than rural regions.

What’s bundled vs. billed separately (quick cost checklist)
When estimating eardrum surgery cost, ask whether these are bundled or separate line items:
- Surgeon fee
- Facility fee
- Anesthesia fee
- Pre-op hearing tests and possible imaging
- Prosthesis/implants (if needed)
- Prescription medications (drops, pain control)
- Post-op visits and repeat hearing tests
A simple way to use this checklist: if you don’t see an item listed in your estimate, assume it may be billed separately until someone confirms otherwise in writing.
Summary: Complexity and what’s “bundled” vs. “separate” are the biggest cost drivers.

Insurance Coverage for Tympanoplasty/Myringoplasty (What’s Usually Covered?)
When insurance is more likely to cover it
Insurance is often more likely to cover tympanoplasty or myringoplasty when it’s considered medically necessary, such as:
- A persistent perforation linked to hearing loss or repeated infections
- Chronic drainage/infection not resolving with appropriate medical management
This “medical necessity” framing is why documentation matters. Your records help connect symptoms, testing, and treatment history to the reason surgery is being recommended.
Common insurance requirements that affect approval and out-of-pocket cost
Many plans look for documentation such as:
- ENT exam notes describing symptoms and duration
- An audiogram (hearing test) demonstrating hearing impact (learn what an audiogram shows in Audiogram Basics: https://sleepandsinuscenters.com/blog/audiogram-basics-explained-a-patients-guide-to-hearing-tests)
- Evidence of appropriate medical therapy when relevant
- Prior authorization
If approval is delayed, it’s often because one of these pieces is missing—not necessarily because the surgery is inappropriate.
In-network vs. out-of-network: the cost difference can be huge
If any part of the surgical team is out of network (surgeon, facility, or anesthesia), patient responsibility can increase substantially. When applicable, out-of-network billing may also raise concerns about balance billing. Confirming network status ahead of time is one of the biggest ways to avoid surprises.
A practical tip: ask specifically about the facility and anesthesia network status—not only the surgeon.
Summary: Medical necessity and network status shape coverage; documentation gets you to “yes.”
Estimating Your Out-of-Pocket Cost (Step-by-Step)
Ask for the right documents (not just a verbal estimate)
If you’re self-pay/uninsured, request a written Good Faith Estimate. If you’re using insurance, ask for a written estimate from the facility and surgeon’s billing offices, plus the insurer’s prior authorization summary (if required). Written estimates make it easier to compare what’s included, spot missing line items (like anesthesia), and track codes if something changes.
Questions to ask your insurance company
- How much deductible do I have left this year?
- What is my coinsurance percentage for outpatient surgery?
- Is there a copay?
- Are anesthesia and implants covered?
- Do I need prior authorization?
This is the most direct way to estimate the cost of tympanoplasty with insurance for your plan. For example, if your plan has a $2,000 deductible remaining and then 20% coinsurance, your out-of-pocket could be shaped far more by your benefits than by the “average price” you saw online.
Questions to ask the surgeon’s office/facility billing
- What CPT/HCPCS codes are expected?
- Based on my exam/testing, is ossiculoplasty possible—and how would that change cost?
- What follow-up visits are included?
If you’re comparing locations, ask whether the estimate assumes a hospital outpatient department or an ambulatory surgery center.
Summary: Your benefits, network status, and a written estimate are the clearest path to a realistic number.
Costs People Forget to Budget For (Hidden or “Add-On” Expenses)
Pre-op costs
Common items include:
- Audiogram/hearing evaluation
- Imaging (CT) in select cases
- Labs if required by the facility
Even small pre-op charges can add up if they hit a deductible, so it’s worth asking which tests are expected and whether they’ll be billed through the facility, an outside lab, or a separate imaging center.
Post-op costs
Budget for:
- Prescription drops/medications
- Transportation and help at home (if needed)
- Time off work and childcare
- Follow-up appointments and repeat hearing testing
These practical expenses are part of the real-world tympanoplasty recovery cost, even when the surgery itself is covered. For many families, time off work is the “largest invisible line item,” even though it doesn’t show up on a medical bill.
If traveling for surgery (medical tourism)
Consider:
- Flights and lodging
- Extended stay if recovery takes longer than expected
- Follow-up care at home and who will manage it
When comparing a bundled package to local care, separate the math into two buckets: (1) the surgical package itself and (2) everything required to make that package workable and safe for you afterward.
Summary: Add-ons and logistics can swing the real total more than people expect.
Treatment Alternatives That May Cost Less (When Appropriate)
Watchful waiting (small perforations)
Some small perforations may heal on their own over time, while others persist. An ENT evaluation helps clarify when observation may be reasonable versus when repair is more strongly considered. If watchful waiting is an option, ask what “success” looks like (symptoms improving, fewer infections, better hearing) and what timeline would prompt re-checking or changing course.
Infection control and ear protection strategies
Reducing infections and preventing water exposure can be part of conservative management in select situations. Sometimes the short-term cost of visits and medications can still be lower than surgery—but the best approach depends on the pattern of infections, drainage, and hearing impact.
Ear tubes or Eustachian tube treatment (for select patients)
Some patients primarily struggle with pressure/fluid problems rather than a persistent perforation. In those cases, different approaches may be discussed. For example, learn about adult ear tubes as an option sometimes used for persistent middle-ear fluid: https://sleepandsinuscenters.com/blog/adult-ear-tubes-in-office-rapid-relief-for-fluid-infections
Clarification: These approaches address related middle-ear pressure/fluid issues and are not one-to-one substitutes for repairing a persistent eardrum perforation.
Summary: Alternatives depend on the problem you’re solving—perforation closure vs. fluid/pressure control.
Lifestyle & Recovery Tips That Protect Your Repair (And Your Wallet)
Water precautions and infection prevention
Many post-op instructions focus on keeping water out of the ear while healing and avoiding trauma (including avoiding cotton swabs). Following post-op guidance may reduce the risk of infection or setbacks that can add cost.
Pressure-change precautions
Activities involving pressure change (like flying/diving) may be restricted for a period of time depending on your surgery and healing. If travel is unavoidable, ask your surgeon’s team for specific timing guidance so you can plan with fewer surprises.
Follow-up adherence
Follow-up visits help confirm healing and address issues early—potentially preventing complications that can increase overall eardrum surgery cost.
Summary: Careful recovery protects both your hearing and your investment.
FAQs
Q: How much does eardrum surgery cost with insurance?
A: It depends on whether your surgeon, facility, and anesthesia are in network, plus your deductible and coinsurance. For some patients, out-of-pocket costs may be relatively limited; for others (especially with high deductibles or out-of-network care), costs can be much higher.
Q: What’s the difference between myringoplasty and tympanoplasty cost?
A: In general, myringoplasty cost is often lower because it’s a simpler repair focused on closing the perforation. Tympanoplasty cost may be higher because it can include additional middle-ear evaluation/reconstruction. Terminology and coding can vary, so confirm how your surgeon defines and bills your procedure.
Q: Why can tympanoplasty cost over $10,000 in the U.S.?
A: U.S. totals can exceed $10,000 due to a combination of facility charges, anesthesia, regional pricing, and case complexity. Facility charge tables list tympanoplasty-related procedures around approximately $10,200 to $20,800 depending on the code and complexity; these are listed charges, not negotiated rates or patient out-of-pocket amounts [1].
Q: Is eardrum surgery covered by Medicare/Medicaid?
A: Coverage is often available when the procedure is medically necessary, but requirements (documentation, prior authorization rules, and patient responsibility) vary by plan and state.
Q: Does a cheaper overseas package include everything?
A: Sometimes packages are bundled, but inclusions vary. Confirm what’s covered for anesthesia, implants/prostheses, follow-ups, and complication care—especially once you return home. These are advertised package prices and may not reflect total end-to-end costs [3].
Q: How do I know if I might need ossiculoplasty too?
A: An ENT may use your exam and hearing tests to assess the likelihood, but in some cases the final decision is made during surgery based on what’s found in the middle ear.
When to See an ENT About Eardrum Repair
Signs you should book an evaluation
Consider an ENT evaluation if you have ongoing drainage, recurrent infections, hearing changes, or you suspect a perforated eardrum. If your main concern is cost, an evaluation can still be valuable because it clarifies which procedure is being discussed and whether alternatives are reasonable—both of which affect the estimate you receive.
What to bring to your appointment
- Prior audiograms/hearing tests (if available)
- A list of medications and allergies
- History of ear infections and prior ear surgeries/tubes
- Insurance information and questions about coverage
If you’d like to request an appointment at Sleep and Sinus Centers of Georgia, you can use this page: https://sleepandsinuscenters.com/appointments
You can also learn more at https://www.sleepandsinuscenters.com/
Summary: A focused ENT visit clarifies diagnosis, treatment options, and what your real costs are likely to be.
Citations
1. VA Outpatient Facility Charge Table (2023) – tympanoplasty-related listed facility charges (approx. $10,200–$20,800 depending on procedure). https://www.va.gov/COMMUNITYCARE/docs/RO/Outpatient-DataTables/v3-27_Table-F.pdf
2. National Friendly Schedule of Fees (2023) – UK private fee schedule examples: Myringoplasty £663; combined-approach tympanoplasty £753. https://nationalfriendly.co.uk/media/tk1bn4xo/schedule-of-fees.pdf
3. Bookimed Turkey Tympanoplasty Pricing (2026) – Advertised Turkey package pricing commonly ~$2,500–$3,200; also cites a U.S. estimate around ~$8,500 (methodology and inclusions vary). https://us-uk.bookimed.com/clinics/country=turkey/procedure=tympanoplasty/
4. NHS England National Tariff Workbook 2022/23 (reference for how national tariffs can structure procedure payments in the UK). https://www.england.nhs.uk/wp-content/uploads/2020/11/22-23NT_Annex-DtA-National-tariff-workbook.xlsx
This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.
Don’t let allergies slow you down. Schedule a comprehensive ENT and allergy evaluation at Sleep and Sinus Centers of Georgia. We’re here to find your triggers and guide you toward lasting relief.








